Having your provider or a nurse call you with news of an abnormal pap smear can be alarming. Knowing something about what pap smears screen for, how often screening is recommended and how to follow up on an abnormal pap can be reassuring if you receive this call.
Why are pap smears important?
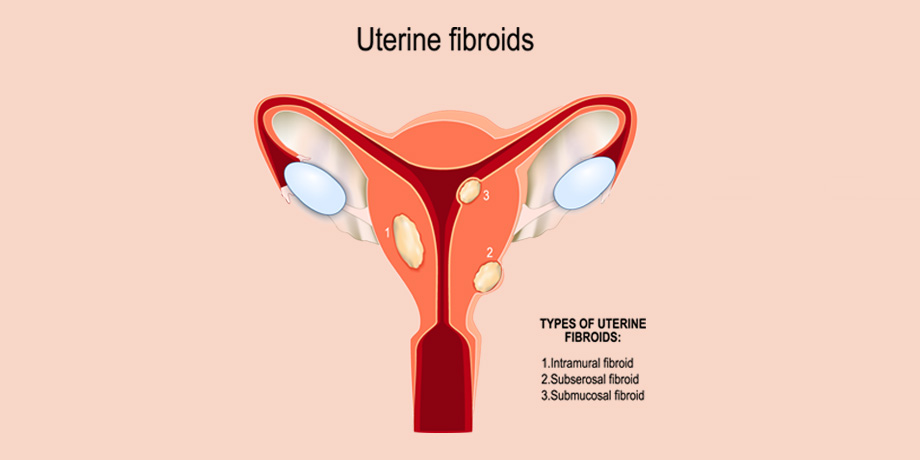
Pap smears are designed to screen for precancerous or cancerous changes on the cells of the cervix in women who are 21 years of age or older. If ordered by your provider additional testing for sexual tract infections (STIs) can also be collected at the same time. As mentioned, paps are a screening tool and if certain abnormal changes are found you will receive further testing.
If you received the Human Papillomavirus (HPV) series of 2-3 vaccines, you have protection from the most common viral types linked to cervical cancer. There are over 150 types of HPV and it is considered to be the most commonly found STI. Of those 150 viral types the two most commonly responsible for cervical cancer are types 16 and 18.
Having the vaccine does not mean that you may skip routine screening pap smears it does mean that you are less likely for low-risk changes to develop into cervical cancer. Early identification of abnormal cells is vital in preventing these cells from developing into cervical cancer.
As a rule, the changes from precancerous to cancerous cells occur slowly over years which is why we can recommend that some low-risk pap results are not re-evaluated for a year while other changes need closer follow up.
Are there risk factors for cervical cancer?
Almost all cervical cancer is caused by the HPV virus. The cellular changes found on pap smears have been studied extensively as have the risk factors related to cervical cancer. The following are known risk factors for cervical cancer:
- Multiple lifetime sex partners
- Smoking
- Having HIV or another auto immune disorder
- Being on birth control pills for 5 years or more (this may be related to multiple sexual partners)
- Certain nationalities with Hispanic and African American women of greatest risk
- Not having received the HPV vaccine
- Not obtaining screening paps or follow-up procedures as recommended
How is the pap smear obtained?
A pap smear is obtained during routine screening at your well woman visit based on age, medical history and previous pap results. After the speculum is inserted into the vagina a small brush is used to gather endocervical cells (cells at the opening of the cervix) and a smooth plastic spatula is used to obtain ectocervical cells (cells at the smooth rounded part of your cervix).
These cells are placed into a specimen container and then sent to pathology. Other than the minor discomfort of a speculum insertion, there should not be pain when obtaining this specimen as there are no sharp instruments used to remove tissue. The specimen is merely sloughed off cells from the cervix.
How often should I get a pap smear?
There are professional organizations that perform most of the research on when paps should be obtained and what follow up is recommend. Your women’s health provider may base their recommendation on those of the American Cancer Society, the American Society of Cytology and Cervical Pathology, the American College of Obstetrics and Gynecologists or other governmental agencies.
It is best to follow those recommendations depending on the results of your pap. Your provider will know these standard recommendations and can explain to you the safest was to manage your results.
Other considerations when deciding how often to get a pap done are whether or not HPV DNA testing was done with the pap. As an example, with a negative pap and no history of abnormal paps the consensus is that you may wait for 3 years to obtain another pap if you are otherwise at low risk for cervical cancer.
If HPV DNA testing was done at the time of the pap, you may even be able to wait for 5 years in certain low-risk woman. However, that does not mean that you go 3-5 years before receiving routine well woman care. Those visits continue to be recommended annually whether or not you are due for pap smear because other important screening is done at those visits.
What is done when a pap is considered abnormal?
The follow up for an abnormal pap could be any of the following:
- A repeat pap in a year
- A colposcopy: an exam done in the office to obtain tissue if suspicious areas of the cervix are identified
- Cryotherapy: an office procedure to freeze cervical tissue which then sluffs off so that new healthy tissue can regrow
- Minor surgical removal of the abnormal tissue expecting that tissue regrowth will be normal
- In rare cases when the cancer has extended beyond the cervix there are other surgical options that would be offered
The best way to take care of yourself is to develop an ongoing relationship with your doctor, midwife or nurse practitioner and follow evidence-based recommendations for all types of health screening.